Obesity and Infertility – Does obesity affect pregnancy?
Obesity and Infertility: Obesity is a life-long, progressive, life-threatening, genetically-related, multi-factorial disease of excess fat storage. BMI (Body Mass Index) = Weight in Kg / Height in M2. For Asian populations, classifications remain the same as the international classification, but public health action points for interventions are set at 23, 27.5, 32.5 and 37.517. Obesity has reached epidemic proportions in India in the 21st century, affecting 10% of the country’s population and another 12% being overweight. 1.5 million deaths are reported due to obesity in 2000 and 20 million deaths due to obesity in 2010.
What is Metabolic syndrome?
Metabolic Syndrome is a condition in which excess body fat is accumulated to such an extent that health may be negatively affected and the life span is shortened. It is a group of diseases where increased abdominal girth more than 90 cm in males and more than 80 cm in females generally associated with increased BMI, diabetes, dyslipidemia, hypertension, polycystic ovarian disease, sleep apnea and non-alcoholic steatohepatitis.
Obesity and Infertility:
How is Obesity related to Infertility? Obesity makes it difficult for women to get pregnant. If they get pregnant, then there is higher risk of losing it. Hormonal levels are also altered in obese women. Obesity related complications in pregnancy (BMI >35): Preeclampsia (5 times), stillbirths after 28 weeks gestation (3 times), early neonatal death (3.5 times), large-for-gestational-age infants (4 times), gestational diabetes (8 times). The infertility treatment including IVF also has lesser success in obese people.
Management of Obesity:
By lifestyle and medical methods weight loss is modest and rarely sustained. We had only few medicines to take care of Obesity. Leucine 2.25 gm with B6 30 mg per day increases fatty oxidation by 30 percent which may help to lose weight to some extent.
Obesity and Infertility – Treatment Options
Non-Surgical treatment: Intragastric Balloon (IGB):
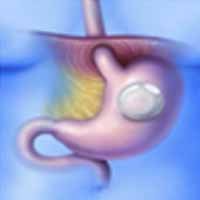
It is placing a deflated balloon in the stomach using endoscope and then filling it to decrease the amount of intragastric space. It can be left in the stomach for a maximum period of six months. It results in average weight loss of 10 to 15 kg. It may be used in patients with overweight who are not suitable for Metabolic Surgery
Surgical Treatment (Metabolic Surgery):
The term “bariatric” surgery is derived from the Greek word baros for weight; defines surgical procedures designed to produce substantial weight loss. Metabolic Surgery – Metabolic changes occurring cannot be explained completely by their effects on body weight alone; hence procedures which induce metabolic improvements come under the category of metabolic surgery.
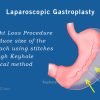
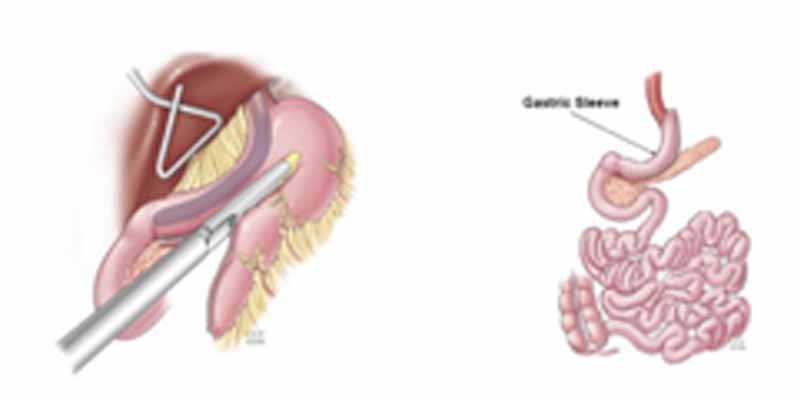
Laparoscopic Sleeve Gastrectomy (more than 30 BMI patients) :
The portion of stomach which secretes Ghrelin and acid in excess is removed. This leads to reduction in food intake and also alteration in hormonal milieu which leads to usage of stored fat for caloric requirement. This has got very good results without significant nutritional deficiency and hence most preferred.
Modified Sleeve Gastrectomy with Ileal Interposition (BMI 25 – 30):
In this after a modified sleeve gastrectomy ileum is brought near the stomach by interposing proximally. The jejunum is connected after ileum. This ensures early entry of food to ileum but jejunum is not kept out of its route. There is significant increase in GLP1 hormone and resultant increase in timely secretion of insulin. There is no dumping or vitamin deficiency in contrast to bypass procedures.



Patients will be initially on liquid diet and later on changed to semi solids, gradually changed to solid diet in a month’s time. Patients will be on vitamins for a month or so, Pantoprazole for 2 months; Calcium will be optional. Biotin is advised if patient has significant hair loss. There is no need for long term vitamins.
RESULTS:
Around 85 to 90 % of diabetes patients treated by these surgeries get complete resolution of diabetes. Whereas, the rest of them get significant control of diabetes with reduced dose of medication. In addition to diabetic control the other benefits are loss of excess weight and control of triglyceride levels. Sleep apnea, arthritis, cardiac episodes, kidney disorders and cancers are also reduced significantly. Studies show that metabolic surgery is cost-effective and safe. IFSO Global Registry studied more than 1 lakh bariatric surgeries over 18 countries and has reported a mortality of 0.03%. SOS – Swedish Obese Subject Study (prospective matched cohort study with 15 years follow up) showed excellent results of metabolic syndrome resolution which is sustained even after many years.
When can pregnancy be planned?
Patients can conceive after 6 months of Bariatric Surgery. Generally, there is no need for any special nutrition or vitamin supplementation to these patients other than what is recommended for a pregnant lady routinely. Bariatric surgery might be effective in young infertile obese women who wish to become pregnant. Weight-Loss surgery resolves PCOS. Most of the improvement in PCOS symptoms occurred during the first 12 months after bariatric surgery.
Conclusion:
Metabolic surgery has emerged as the most preferred, highly effective, and safer means to achieve long term resolution of type 2 diabetes and excellent improvement in fertility status.
Video Talks on Bariatric Surgery
| Topic | Watch |
|---|---|
| Intragastric Balloon Placement This balloon is enough to reduce 15 kg weight in days | Watch video |
| Talk by Dr. R. Padmakumar on World Obesity Day | Watch video |
| Diabetes and Obesity - Malayalam October 4, 2019 | Watch video |
| Keyhole Surgery and Obesity January 2019 | Watch Video |
Video Testimonials
| Testimonial | Watch |
|---|---|
| Ramesh Kumar presents his Bariatric Journey to wellness - From 157 Kg to 102 Kg in 1 year | Watch Video |
| Weight Loss from 138 Kg to 108 Kg in 3 months. Patient shares his experience from Oman | Watch Video |
| Weight Loss from 157 kg to 113 kg after Sleeve Gastrectomy. Patient shares experience of Sugar level coming down to normal condition after the surgery. 22 Kg weight loss in the first month itself. | Watch Video |
| Weight Loss after Bariatric Surgery from 85 Kg to 60 Kg. Cholesterol got normal, leg pain resolved | Watch Video |
| Weight Loss after Sleeve Gastrectomy - after One Year 130 kg to 80 kg. Had trouble breating, snoring before the surgery due to obesity. After surgery, snoring and trouble breathing has resolved. | Watch Video |
| Weight Loss after Bariatric Surgery April 2019 | Watch Video |
About Dr. R. Padmakumar
Dr. R. Padmakumar is one of the Best Hernia Surgeon in India. He has been changing lives through Keyhole Surgery. He has got more than 30 years of hands-on experience in laparoscopic Surgery in major hospitals across India and has completed more than 7000 cases of Laparoscopic Hernia Surgeries. Dr. Padmakumar has trained more than 300 surgeons from all over the world the art of laparoscopic surgery especially Laparoscopic Hernia Surgery. Dr. Padmakumar is also hailed as one of the Best Bariatric Surgeon in India & UAE. He is renowned for new and improved treatment techniques and the first in the World to perform Scarless Bariatric Surgery with Tummy Tuck / Abdominoplasty. He is also one of the very few thyroid surgeons in India doing Endoscopic Thyroidectomy (scarless thyroid surgery).


-
Anal Fissure Treatment
-
Gynaecomastia Treatment
- Piles / Hemorrhoids Treatment
- Varicose Veins Treatment
- Laser Treatment for Varicose Veins
- Diabetic Foot Treatment