Type 2 Diabetes Surgery

Type 2 Diabetes Surgery – Type 2 diabetes mellitus (T2DM) is a common disease associated with numerous complications. Obesity is the leading cause of the increased incidence of type 2 diabetes mellitus in both developed and developing countries. Obesity and overweight have in the last decade become a global problem – according to the World Health Organization (WHO). There are many risk factors for type 2 diabetes.
It is an astonishing fact that the number of people having Diabetes Mellitus (DM) is increasing day by day. Asians have higher incidence of Diabetes, due to genetic reason. Life style changes and food habits contribute to this increase. Diabetes affects all organs in the body like eye, brain, heart, kidney & limb vessels. These lead to early death.
- Heart attack at an early age
- Stroke
- Kidney disease leading to kidney failure, which may require dialysis. 45% of dialysis patients are contribution of diabetes.
- Nerve damage which can lead to digestive and bladder problems sexual dysfunction and numbness or tingling in the legs.
- Foot problems including ulcers and poor circulation that can lead to amputation.
- Eye complications such as glaucoma, cataract, and retinopathy, that can lead to blindness
International Diabetic federation has approved bariatric surgery as preferred and effective treatment of diabetes; benefits of surgery being long lasting remission of diabetes; control of other associated illnesses and cost effectiveness.
NEJM (New England Journal of Medicine) rates metabolic surgery to cure Diabetes as the most important innovation of 2012.
Keyhole Surgery for Type 2 Diabetes Resolution
Type 2 Diabetes is the result of
- Increased demand for insulin due to higher quantity of food eaten.
- Reduced production of insulin due to fat deposition in pancreas or pancreatic cell hypo function
- Glucose supply from liver (neoglucogenesis) due to fatty liver and
- Most importantly insulin resistance (the insulin available in the body is not able to take care of the glucose due to excess fat in the body).
It is now clear the intestinal hormone (GLP1) levels can regulate the insulin production in pancreas. Hence by increasing GLP1 level in the gut, diabetes can be controlled. GLP1 is produced in large quantities by terminal portion of small intestine. Partially digested food reaching this region increases the production of this hormone. There are other neurohormonal gut mechanisms as well, working in favour to control of diabetes.
By keyhole surgery the stomach size is brought down hence excess food intake will be reduced and gastric emptying is accelerated. Last portion of small intestine is brought towards the stomach that helps in bringing partially digested food into the small intestine rapidly, thus increasing GLP1 level and there by increasing insulin levels. Obese diabetics require modified sleeve gastrectomy alone while non obese diabetics require sleeve gastrectomy and ileal interposition. The weight reduction and associated fat loss will also increase insulin activity. These surgeries are found to increase insulin performance and give long standing resolution of diabetes.
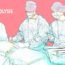
Keyhole Surgeries for Resolution of Obesity
Laparoscopic Sleeve Gastrectomy ( > 30 BMI Patients).
Laparoscopic Gastric Banding.
Modified sleeve gastrectomy & Ileal Interposition (25 to 30 BMI patients).
Intragastric Balloon for Weight Reduction
Click here to Read on Intragastric Balloon Placement.
Minimally Invasive Hybrid Surgery for Ileal Interposition
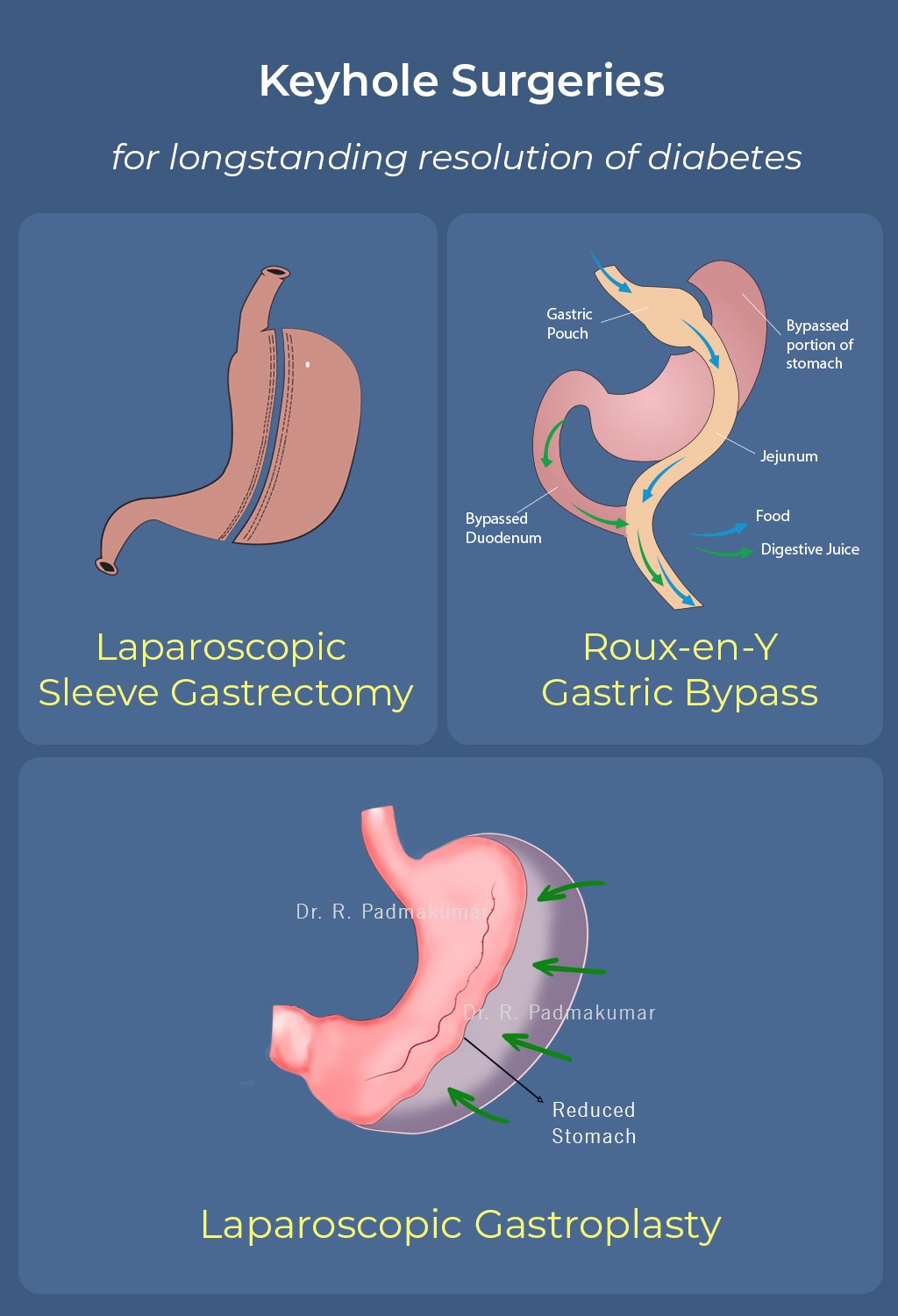
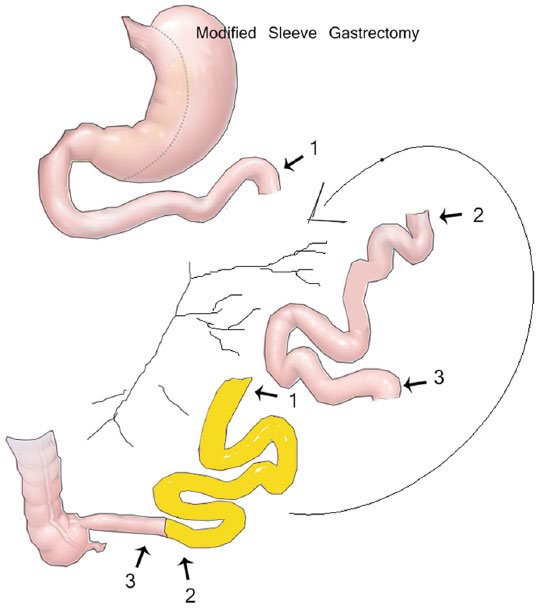
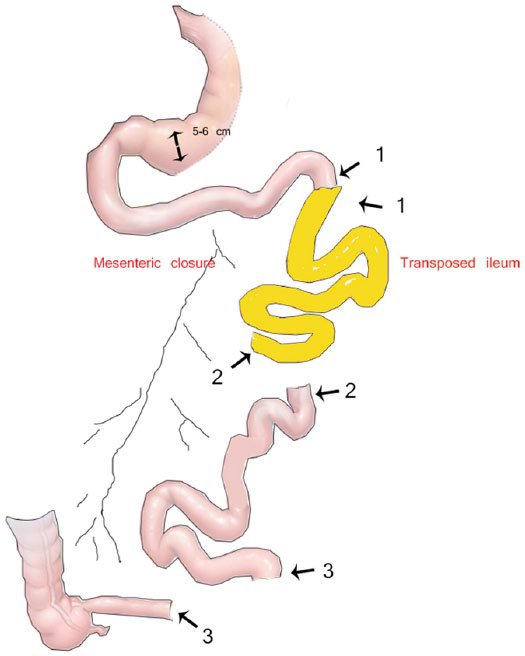
MIHSII is an innovative technique in which sleeve gastrectomy is performed laparoscopically, followed by extracorporeal ileal interposition performed through a 5-cm midline incision. MIHSII is a cost-effective and minimal procedure for the resolution of T2DM in patients with BMI <30 kg/m2.
MIHSII Procedure diagram


Is Type 2 Diabetes Surgery feasible for you?
These procedures are helpful in patients with Type 2 diabetes, in whom pancreas is capable of producing good level of insulin. These are having much better result in those with more than ideal weight and in those with diabetes of shorter duration (few years) than in those who have already damaged their end organs like kidney, eye, heart, etc. So it is better to undergo this procedure before pancreas fails significantly and before end organs damage starts. It is highly appreciable for a diabetic patient to know that cure is possible. In Type I diabetes (where pancreas is not functioning at all or has antibodies against insulin) these surgeries are not helpful.
85% to 90% of diabetic patients treated by these surgeries are cured of diabetes. Other 10 to 15% also could reduce their medications significantly. In addition to diabetic control the other benefits are loss of excess weight and control of cholesterol, sleep apnoea, joint pains, cardiac disease, hypertension, kidney disorders, eye problems etc. It definitely improves quality of life and reduces cancer risk, infertility & mortality (early death).
All these procedure are done under general anaesthesia and patient will be observed for 4 days in hospital. These are done by laparoscopic and minimally invasive methods using equipments like staplers & harmonic scalpel. Hence, patients will be highly comfortable and can resume normal activity in a few days time.
About Dr. R. Padmakumar
Dr. R. Padmakumar is one of the Best Hernia Surgeon in India. He has been changing lives through Keyhole Surgery. He has got more than 30 years of hands-on experience in laparoscopic Surgery in major hospitals across India and has completed more than 7000 cases of Laparoscopic Hernia Surgeries. Dr. Padmakumar has trained more than 300 surgeons from all over the world the art of laparoscopic surgery especially Laparoscopic Hernia Surgery. Dr. Padmakumar is also hailed as one of the Best Bariatric Surgeon in India & UAE. He is renowned for new and improved treatment techniques and the first in the World to perform Scarless Bariatric Surgery with Tummy Tuck / Abdominoplasty. He is also one of the very few thyroid surgeons in India doing Endoscopic Thyroidectomy (scarless thyroid surgery).


-
Anal Fissure Treatment
-
Gynaecomastia Treatment
- Piles / Hemorrhoids Treatment
- Varicose Veins Treatment
- Laser Treatment for Varicose Veins
- Diabetic Foot Treatment